Best Home Blood Pressure Monitors for Accurate Readings
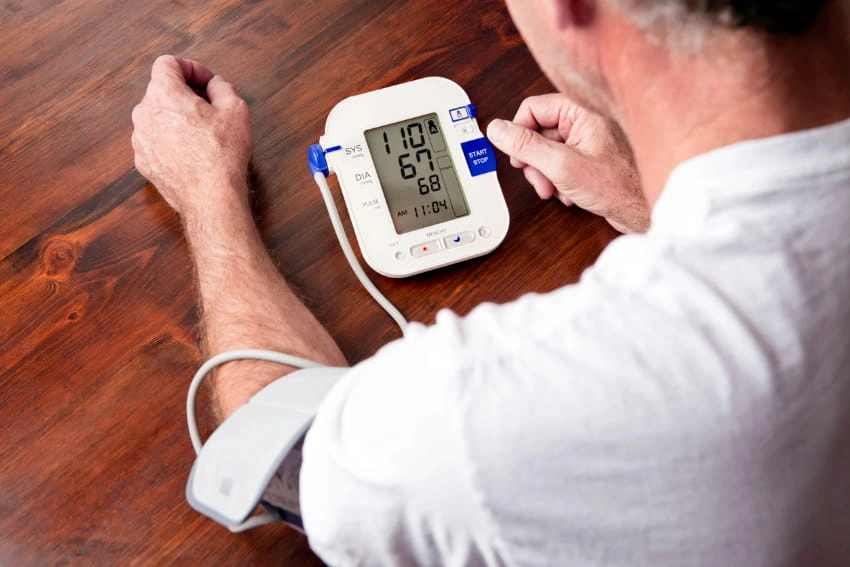
Best Home Blood Pressure Monitors for Accurate Readings | Monitoring heart health is no longer a task confined to clinics or hospitals. With significant advancements in medical technology, tracking your blood pressure independently has become a highly recommended preventive measure for people of all ages. One of the most essential instruments for every modern household today is the digital tensiometer. This device allows individuals to detect early signs of hypertension—often called the “silent killer”—without requiring professional medical expertise or frequent trips to the doctor.
Why Choose the Upper Arm Type Over Wrist Models?
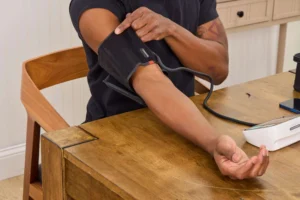
When deciding to purchase a blood pressure monitor, you will inevitably encounter two primary types: wrist monitors and upper arm monitors. Although wrist models appear more compact and offer better portability for travelers, health experts and medical practitioners strongly suggest using the upper arm type for primary home use.
The reason for this preference is simple yet critical: accuracy. The anatomy of the upper arm allows the cuff to be positioned naturally at the same level as the heart. This alignment minimizes the risk of reading errors that often occur with wrist monitors, which are highly sensitive to even slight changes in body positioning or arm height. By obtaining more stable and consistent readings, the data you collect serves as a much more valid reference when you need to consult with a physician or adjust your daily lifestyle habits.
Evaluating Quality, Brand Reputation, and Pricing
Investing in a health device requires a careful balance between quality, reliability, and cost. In the medical device industry, trusted brands like Omron have long been considered the gold standard due to their long-term durability and clinical precision. For home users, popular models such as the Omron HEM-7142 or the M2 Series are exceptionally practical choices that bridge the gap between professional performance and user-friendly design.
Generally, these high-quality devices are priced competitively between 37 to 70 USD. In many markets, this price range ensures that the device has undergone rigorous clinical validation and carries recognized medical certifications. While cheaper, generic alternatives might be tempting, investing in a reputable brand provides the peace of mind that the numbers you see on the screen are reflective of your actual health status rather than a technical glitch.
Advanced Features for Comprehensive User Convenience
Modern digital monitors do much more than just display systolic and diastolic numbers. To stay competitive and helpful, they often include several integrated features that help you monitor your cardiovascular condition more comprehensively:
-
Irregular Heartbeat Detection: This is a vital safety feature. The device alerts the user if the sensor detects an arrhythmia or any irregular heart rhythm during the measurement process, which could be an early warning sign of underlying issues.
-
Internal Memory Storage: Gone are the days of manually recording every result on a piece of paper that eventually gets lost. Most modern devices can store dozens or even hundreds of previous measurements, complete with dates and timestamps, allowing you to track trends over weeks or months.
-
Cuff Wrap Guide: One of the most common mistakes in home testing is improper cuff placement. This feature provides a clear visual signal (often a green light or icon) to confirm that the cuff is wrapped correctly and not too loose.
Expert Tips for Achieving the Most Accurate Results
To get the most out of your digital device and ensure your data is reliable, follow these medical best practices:
-
Rest and Calm Down: Sit quietly without distractions for at least 5 minutes before starting the test. Avoid smoking, caffeine, or heavy exercise for 30 minutes prior.
-
Maintain Correct Body Posture: Sit upright in a chair with your back well-supported and your feet flat on the floor. Do not cross your legs, as this can temporarily raise blood pressure.
-
Position Your Arm at Heart Level: Rest your arm on a flat surface like a table. The cuff on your upper arm should be at the same horizontal level as your heart.
-
Practice Consistency: Take two or three measurements with a 1-2 minute break in between. Calculate the average of these readings to get a more stable representation of your pressure.
A Small Investment for Long-Term Peace of Mind
Owning a digital blood pressure monitor at home is an act of proactive care for yourself and your loved ones. With a relatively affordable investment, you gain access to an accurate diagnostic tool like the Omron HEM-7142 that empowers you to take charge of your wellness. Monitoring your blood pressure regularly is not about being paranoid or feeling “sick”; rather, it is a conscious, modern effort to ensure your cardiovascular system functions optimally in the long run, helping you live a longer, healthier life.